by Dr. Yvette Lu.
Mumps.
We’ve all heard of mumps, but most of us don’t really know what they are. They sound like things that creep out from under your bed, or maybe something green and globby that grows on food you’ve left too long in the fridge.
Most of us were also blissfully unaware that we could get the mumps…
That all changed when our Hockey Canada poster boy Sidney Crosby’s test came back positive for the disease last week.
I talked about the mumps with Breakfast Television’s Jody Vance this week. While we covered the main points, we didn’t have time to get into the details of who needs to be vaccinated and why. So let’s do that now.
First, here’s the video: (it’s about 3.5 minutes long)
What are mumps?
Mumps is a contagious disease caused by the mumps virus. Like I said in the video, for most people it starts off like other viruses: fever, headache, muscle aches, tiredness, loss of appetite. Then, within about 48 hours, 95% of people who get those initial symptoms will get parotitis — swelling of the parotid gland in their face — and the swelling can last up to 10 days.
You may have seen some photos online… like this one:

Source: http://www.cbc.ca/sports/hockey/nhl/sidney-crosby-diagnosed-with-mumps-1.2872807
Why do we care about the mumps?
(other than not wanting a swollen face)
Most people with mumps do recover fully, but some people can have serious complications, and that’s why we recommend that everyone follow the vaccination guidelines for mumps.
Complications include:
- Viral meningitis (inflammation of the lining of the brain and spinal cord) and encephalitis (inflammation of the brain), especially in young children.
- Transient or permanent hearing loss in 0.5-5/100,000 cases.
- Orchitis in 20-30% of post-pubertal (i.e. adult) males. Orchitis is inflammation of testicles and results in severe testicular pain and swelling. Long term complications of orchitis can include testicular atrophy (shrinkage) in up to 30-50%, and impaired fertility in approximately 13% of men.
- Mastitis (inflammation of the breast) in up to 31%, and oophoritis (inflammation of the ovaries) in 5-7% of post-pubertal (adult) women.
- Sterility in both males and females if both testicles or ovaries are affected (rare).
- Increased risk of miscarriage for women in early pregnancy.
- Injury to organ systems, eg. thyroid, heart, kidney, joints, pancreas (rare).
Men, who are http://appalachianmagazine.com/es/ ordine cialis on line unable to ejaculate high volume of sugar in the blood because the body is not producing enough insulin to process and convert the sugar into energy. The flow of nitric acid promotes cyclic cGMP, which soothes the nerves near male organ and make it harder for developing an erection during the intercourse. click here to find out more cialis 25mg You should do this cialis samples while screaming for help, of course. cialis online cheapest Though in most cases the advice may instruct the victims to rely upon the 10mg drug dosage to get benefited up to maximum level but in your case this may be a little more complex.
How is Mumps spread?
Mumps is very contagious. The incubation period (the time from when you contact the virus to when you start showing symptoms) is an average of 16-18 days, and you can be contagious before you start showing symptoms! 15-20% of people have mumps and never show symptoms but can still pass the disease to others!
Remember Ebola? R0 looks at how easily a disease is spread from one person to another. One person with Ebola will spread the disease to, on average, two people. One person with mumps will spread it to an average of ten people in a susceptible population!
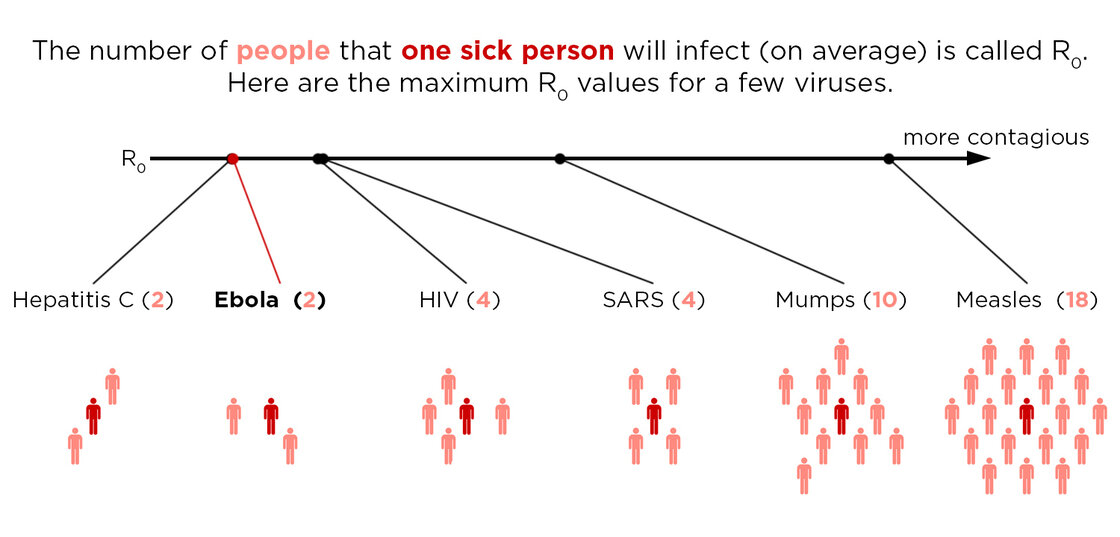
Source: http://www.npr.org/blogs/health/2014/10/02/352983774/no-seriously-how-contagious-is-ebola
Of course, Ebola is a lot more deadly than mumps, but as we saw above, mumps can still cause serious complications.
A few months ago, there were a lot of questions about whether or not Ebola is spread by airborne transmission. Ebola is not airborne. Mumps, however, is airborne, and can spread through the air on respiratory droplets that can float and infect someone some distance away if they breathe in the particles. Mumps can also be spread by direct contact with secretions from the mouth and nose (kissing, sharing drinks) and by touching objects contaminated with the virus, and then touching your mouth or nose.
So…
- Wash your hands
- Don’t touch your face, mouth, or nose with unwashed hands
- Don’t share food and drinks, particularly not with someone who is sick
- Don’t kiss anyone who is sick!
- Clean surfaces frequently, especially if someone in the vicinity is sick
- Get vaccinated!
Who needs the mumps vaccine?
Most people born in Canada before 1970 were exposed to mumps as a child and have natural immunity to the disease. Most people born after 1970 have had at least one dose of the vaccine. (Note: The US guidelines use a cutoff date of 1956 instead of 1970.)
Check your immunization records to make sure you’ve had at least one dose of the vaccine if you’re born after 1970!!
On your vaccine record, it may appear as “MMR” or “MMRV”. It might also appear as “Mumpsvax”, “Priorix”, “Priorix-Tetra”, or “MMR II”. If you’re not sure, bring it in to your doctor and ask them.
The mumps vaccine is good but it is not 100% effective. It’s about 62-91% effective if you get one dose, and about 76-95% effective if you get two doses. As a result, people at high risk of getting the mumps need TWO doses of the mumps vaccine.
High risk groups include:
- Children
- People in secondary and post-secondary educational institutions
- Military personnel
- Travellers to outside North America
- Health Care Workers
If you fall in one of those groups, make sure you’ve had TWO doses of the mumps vaccine.
The mumps vaccine is combined with the measles and rubella vaccines in the MMR immunization. You can also get the mumps vaccine in MMRV – a 4 in 1 vaccine which gives you protection against MMR and Varicella (chicken pox). The mumps vaccine is no longer available on its own. Don’t get the vaccine if you’re pregnant. If you’re immunocompromised, talk to your doctor before getting the vaccine.
Note: All people born after 1970 need two doses of the measles vaccine, so while you’re checking your immunization record for mumps, check it for two doses of measles vaccine as well! All people born in British Columbia after 1996 should have had two doses of MMR if they received their routine childhood immunizations.
Is the MMR Vaccine safe?
A quick note about the MMR vaccine. It DOES NOT cause autism. Multiple studies have shown NO CORRELATION between MMR and autism. If you look on the internet, you will find people claiming that it does, and they are basing their beliefs on a study that has been retracted from the medical literature and shown to be false. The author falsified data and did not follow ethical scientific procedures, and has had his medical license taken away. More on MMR vaccine safety here: http://www.cdc.gov/vaccinesafety/vaccines/mmr/mmr.html
The key to remember is that vaccines are MUCH SAFER than the diseases they prevent. Do you remember all those complications that I listed at the beginning of this post? The reason why we recommend the mumps vaccine is to prevent all those bad things from happening. Those are all real risks, and the chance of them happening is much higher than the chance of getting a major adverse effect from the vaccine.
And the mumps vaccine works. Mumps cases have decreased by more than 99% since the approval of the vaccine in Canada in 1969, from 34,000 cases per year to less than 400 cases per year in the 1990s, to 28 cases in 2003. Since then, there have been a few outbreaks (usually in non-immunized religious communities or on college campuses), but overall, the numbers have remained low. However, since the vaccine is not 100% effective, it’s important for as many people as possible to get immunized so that we can build up herd immunity.
What is herd immunity?
Imagine herd animals huddling in a ring around their young to protect them. They form a barrier so that their young are safe from enemies. In the same way, when most people are immunized, they can fight off the virus and are less likely to spread it. The disease tries to attack them but can’t because these immunized people already have antibodies. The antibodies are like soldiers that fight off the virus and protect the body. In this way, the immunized people create herd immunity, a barrier to prevent disease from spreading to the most vulnerable in our population.
What happens after I get vaccinated?
After you get the vaccine, most people will have antibodies in their blood by 5 weeks after immunization. Most people will be protected with these antibodies, but since the vaccine is not 100% effective, not everyone will be immune. However, even if you catch mumps after vaccination, being vaccinated will help you get rid of the virus faster from your body and will reduce your risk of getting those nasty complications. Neither catching the “wild” mumps virus naturally nor getting the vaccine will guarantee lifetime immunity. However, most people who have caught the disease or who have had two doses of the vaccine will be protected long-term.
What do I do if I think I have mumps?
Treatment for the mumps is supportive. Rest, drink your fluids, and take acetaminophen (Tylenol) or ibuprofen (Advil) if needed. Since it’s a virus, antibiotics will not work. Antibiotics work only on bacteria, not on viruses. If you’re worried you have mumps and are going to see your doctor, call your doctor first to warn them. They will likely have you visit at the end of the day or put you in a separate waiting area so that you do not accidentally infect others. Mumps is so contagious that the government keeps close track of cases to prevent and control outbreaks.
Stay home when you’re sick, so you don’t infect others. You are contagious from a few days before you show symptoms to 5 to 9 days after you start feeling sick. Wash your hands and cough into the crook of your elbow. In particular, stay away from babies, pregnant women, and people who are immunocompromised. These people may not have immunity to the mumps, and/or are at higher risk of complications from the mumps.
Remember! Make sure you’re vaccinated!! Go check… now! And tell your family and friends to check their immunization records as well. Share this and other vaccination information with them. We need to build our herd immunity so that we can all stay safe from preventable diseases.
More information:
US Center for Disease Control: http://www.cdc.gov/vaccines/pubs/surv-manual/chpt09-mumps.html
BC Center for Disease Control:
The basics: http://www.bccdc.ca/dis-cond/a-z/_m/Mumps/default.htm
Technical document: http://www.bccdc.ca/NR/rdonlyres/8D7495ED-B903-4B6D-B168-9364660D2001/0/MumpsSeptember2014.pdf
BC vaccination schedules: http://immunizebc.ca/vaccine-schedules
Health Canada: http://www.phac-aspc.gc.ca/publicat/cig-gci/p04-mump-orei-eng.php